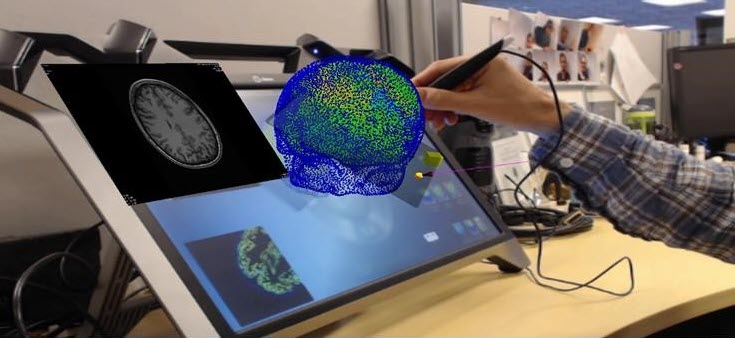
What if it were possible for physicians to virtually analyze their patients’ health and simulate treatments or surgery using the same advanced technology that automotive engineers use to crash-test cars before they are built? What if medical devices and pharmaceuticals could be designed and safely tested virtually, at a fraction of the time and cost required by safety considerations in the real world?
These scenarios could be possible – and sooner than you might think – thanks to the advancement of virtual twin technology, applying knowledge developed in the non-organic world of manufacturing to the challenges of organic life. In fact, significant progress has already been made in creating virtual twins of humans, starting with a variety of major human organs.
At the heart of the matter
The Living Heart Project, for example, launched in 2014, has brought together cardiovascular researchers, educators, medical device developers, regulatory agencies and practicing cardiologists to develop a highly accurate and fully functioning digital model of the complete human heart – and apply it to improving outcomes for actual human patients.
Dr. David Hoganson, a doctor of medicine, assistant in the Department of Cardiac Surgery and director of the Computational 3D Visualization Program at Boston Children’s Hospital in Massachusetts, is already seeing huge benefits of the project. “We are able to create patient-specific models from the segmentation of actual 3D images, either from CT scans or MRIs,” he said. “Using these models, physicians can simulate the blood flow under different conditions – during anesthesia, or after food and/or exercise for example.”

Surgeons at Boston Children’s Hospital also have used the technology to plan an operation virtually – ensuring the right approach is chosen prior to actual surgery. “And that’s not all: the models are proving to be incredibly useful for education,” Hoganson said. “Paper drawings do not do justice to the complexity of heart diseases but, until recently, these are what we have used to teach a patient’s family about their condition and necessary procedures. It is much easier with a 3D model. Now parents can even put on 3D glasses and interact with holographic representations of their child’s heart.”
Meanwhile, Cristina Pop, a clinical research assistant at McGill University in Montreal, is using the living heart model to understand the impact of COVID-19 on people with heart conditions.
“COVID-19 presents a higher risk of severe cardiovascular complications, such as cardiac arrhythmia and heart failure,” Pop said. “At the same time, people with existing cardiovascular diseases are at higher risk of severe illness and death from COVID-19. To understand disease progression, and identify patients at higher risk of cardiac complication, we modeled a number of patients with underlying conditions. The beauty of 3D modeling is that this can be done in a non-invasive way, and with great accuracy. We have been able to simulate, with acceptable accuracy, heart failure progression and develop a better picture of patients’ cardiac status.”
“We are able to create patient-specific models from the segmentation of actual 3D images, either from CT scans or MRIs.”
Dr. David Hoganson, Boston Children’s Hospital
Belgian digital health tech firm FEops, meanwhile, developed a digital twin-based pre-operative planning platform for structural heart interventions.
“Physicians traditionally rely on medical imaging to make decisions on where to place implants and what size to use,” said Matthieu De Beule, FEops’ CEO. “This is an inefficient process, requiring time-consuming preoperative planning – and potentially resulting in sub-optimal implant size and position. There’s logically a big risk of complication if things go wrong. Our solution, using virtual representations of individual patients’ hearts, has far greater accuracy and has the potential to reduce both pre-operative planning and procedure time.”
FEops pre-operative planning platform for structural heart interventions is based on a virtual twin. (Video © FEops)
Building on success
The Living Heart Project demonstrated the power of the virtual twin to combine and apply cross-disciplinary experience – creating a path to virtually model other organs and systems in the body, starting with the brain and then moving to the lungs.
Successful modeling of the brain has facilitated work by India-based technology company BrainSightAI.
“Using virtual representations of individual patients’ hearts has far greater accuracy and has the potential to reduce both pre-operative planning and procedure time.”
Matthieu De Beule, CEO, FEops
“One in six people suffers from brain-related disorders around the world – at a projected cost of $16.3 trillion between now and 2030,” said Laina Emmanuel, BrainSightAI’s CEO and co-founder. “That’s a higher cost than cancer and even chronic respiratory diseases. Brain-related disorders are often a race against time, and long-term hospitalization rates are high.”
Virtual brain models, however, offer significant possibilities, Emmanuel said. “Using resting-state MRI scans, we can design, calibrate and validate brain models to explore the interplay of structural and functional contributors to brain disorders. It’s non-invasive, so very apt for non-cooperative patients such as those in a coma. When teamed with artificial intelligence, we are building a new paradigm for diagnosis and treatment.”
Mona Eskandari, assistant professor of Mechanical Engineering and the BREATHE center at the University of California, Riverside, sees potential in creating virtual models of the human lung.
“COVID-19 in particular has revealed the vulnerable underbelly of lung mechanics; but even before that, lung fatalities were a major cause of morbidity and mortality worldwide,” Eskandari said. “Diagnoses of lung conditions often come down to trial and error, despite early prevention and intervention being key to improving patient outcomes. Moreover, lung diseases cost billions in the US alone.”
Building on the Living Heart Project by replicating its success with human lungs could save lives and significantly reduce these burdens, she said.
“By mirroring the Living Heart Project to focus on the lungs, we can understand where particles from inhalers land, for example. We can understand the pressures put on the lung by ventilators – helping us to devise optimal ventilation strategies informed by tissue mechanics. And as in our recent investigations, we can also understand the continuous evolutionary behavior of a lung and compare local measures with global mechanics.”
Toward the virtual human
Great strides also have been made in using virtual twins to model other parts of the body, including kidneys, feet, skin, cells and the digestive tract. Researchers hope that, over time, these separate models could be combined to create a complete virtual human. They also dream of cohort models – an approach that follows a selection of patients with a shared characteristic over a period of time – defined at the population level. When combined with machine learning, these models could inform novel approaches and help patients get the best available treatment for their specific genetic makeup.
Virtual clinical trials for new medical device designs are just one possible application for such a “system of systems.” The US Food and Drug Administration (FDA) is beginning Year Two of a five-year project that will culminate in an in silico clinical trial using the Living Heart model to create a focus group of virtual patients.
“Their goal is to define a new, more efficient method to achieve regulatory approval, while reducing the burden on animal and human testing,” said Hoganson of Boston Children’s Hospital. “It has the potential to reduce human trials from years to days. It has been a tremendous effort so far – and we are excited about the future.”

The result is a new digital process, which is intended to be more efficient and less expensive than current ones – which involve lengthy patient selection, recruitment and retention together with cumbersome managing and monitoring processes, and often result in delays and costs which can impede patient access to novel treatments – without losing rigor or confidence in a device’s safety and efficacy.
“Modeling and simulation can help to inform clinical trial designs, support evidence of effectiveness, identify the most relevant patients to study, and assess product safety,” said Tina Morrison, Deputy Director in the Division of Applied Mechanics, Office of Science and Engineering Labs, Center for Devices and Radiological Health, FDA in a press release. “In some cases, in silico clinical trials have already been shown to produce similar results as human clinical trials.”
And this is just the start. The experts believe that the sum of these projects has become a showcase example for the transformative power of the virtual twin for healthcare. No longer do they question ‘if’ it is possible to create realistic virtual physiological human models, they ask ‘how’ and ‘when.’
The transformational power of digital
The ultimate goal? To bring a renaissance to clinical care.
“The vision behind creating a virtual twin of a human is to advance the development of personalized medicine,” said Natacha De Paola, professor of Biomedical Engineering at the Digital Medical Engineering & Technology Research and Education Center at Illinois Tech.
The logic is clear. Current methods for analyzing a patient’s health and planning the best therapies and surgeries are time-consuming, error-prone and expensive. They often involve several specialists and technicians across many sectors to plan, execute and manage the patient’s care. In most cases, those experts are limited in their ability to share a full picture of the patient’s situation. By bringing all these stakeholders and key components together in the virtual world, via a virtual human, silos will fall and collaboration will improve.
“We are heading for a fully digitalized healthcare system that sees a virtual twin complementing electronic medical records and serving as a guide for precise and individual treatment,” De Paola said. “To get there we will need to continue to bring together research communities, device and drug development companies, clinical care teams and citizens. We need a skilled and agile workforce, teamed with multi-scale, multidimensional and multifunctional systems.”
While the goal is ambitious – almost daunting – De Paola is confident the medical profession has enough determination to reach it.
“2020 was a transformational year, engineering a number of huge breakthroughs,” she said. “The Living Heart Project opened the door to not only the Living Lung and the Living Brain, but to models of many elements of human physiology. But it’s just the beginning. Now it’s time to open the door to the digital human.”
Discover more about the potential of virtual twins of humans